Workshop
Designing Future State to Account for Social Risk in CMS Payments
January 11, 2021
This invitation only workshop is a one, full-day brainstorming event to design a future state CMS payment system that incorporates social risk in a sustainable, equitable way. This convening of CMS, ASPE, safety net health plan, clinician, state, and patient stakeholders provides the unique opportunity to collaboratively design potential new approaches to risk adjustment for the Medicare and Medicaid programs.
SUMMARIZE
current approaches that successfully incorporate social risk into healthcare payments in the US and abroad.
.
IDENTIFY
creative approaches to incorporate social risk into healthcare payments for CMS.
.
DEVELOP
action items to more deeply explore and potentially operationalize incorporation of social risk into healthcare payments for CMS.
CODIFY
learnings and diffuse them within HHS and broader healthcare ecosystem through a peer-reviewed journal or conference presentation.
Why this is important
Amix of social and economic factors collectively labelled the social determinants of health (SDOH) have a greater combined influence on the morbidity and mortality of our patients than the services we deliver in traditional medical care. Addressing SDOH can prevent illness and unnecessary services and produce better health. And yet, U.S. health care payments do not typically adjust for these factors to support related needs and services and do not support teams or delivery redesign needed to adequately address SDOH. Therefore, clinics that serve patients with disproportionately higher SDOH needs have significantly higher resource demands and require significantly higher reimbursement. The current reimbursement scheme based on Hierarchical Condition Category (HCC) risk adjustment does not take into account SDOH and perpetuates systematic disparities for the most vulnerable patients and the health plans that serve them.
The 2014 IMPACT Act directed the US Secretary of Health & Human Services to review the evidence linking social risk factors with performance under existing federal payment systems and to suggest policy options. Most US states now require assessing and addressing social determinants in Medicaid contracts but most of these offer insufficient specificity or adjustment tied to accountability. And while there are several research studies and philanthropic demonstrations focused on addressing social determinants, there is little U.S. evidence available on which to build. Other countries, including England and New Zealand, have for decades routinely adjusted payments for health care and social services to account for neighborhood deprivation. These international examples, and related models in the US, have the potential to improve the effectiveness of value-based purchasing and health for the nation. There are several, related small-area SDOH indices in the US with a growing amount of evidence of their relationships to important health outcomes, avoidable hospitalizations, and disease prevalence. These indices are potential candidates for meaningful and reliable health services payment adjustment and the second letter to Congress in response to the 2014 IMPACT Act acknowledges that area-level SDOH indices may be a viable way to adjust resources to providers.
Implications for policy action
Consideration of small-area based SDOH indices as a mechanism for payment and quality measure adjustment in response to the 2014 IMPACT Act. Small-area based SDOH indices can also be used as a mechanism for health system and /or neighborhood-level resource allocation, for individual patient-level resource allocation, programmatic targeting , and service eligibility determinations. This latter point can be especially important in promoting increased efficiencies for front-line providers in service-outreach efforts. Precision-Level geographic approaches like these can also naturally enhance synergy and collaboration amongst the multitude of federal, state, local and private agencies that address social determinants of health.
Medicare FFS – CMMI Model
Social risk factors incorporated into risk-adjusted payments for some Medicare FFS providers that are part of a CMMI model
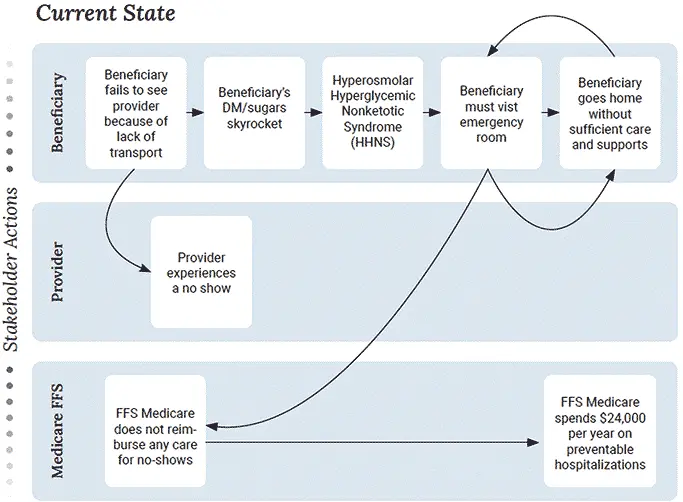
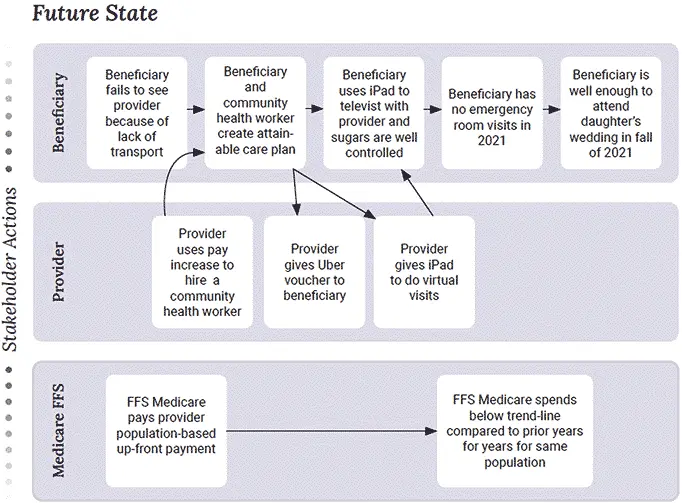
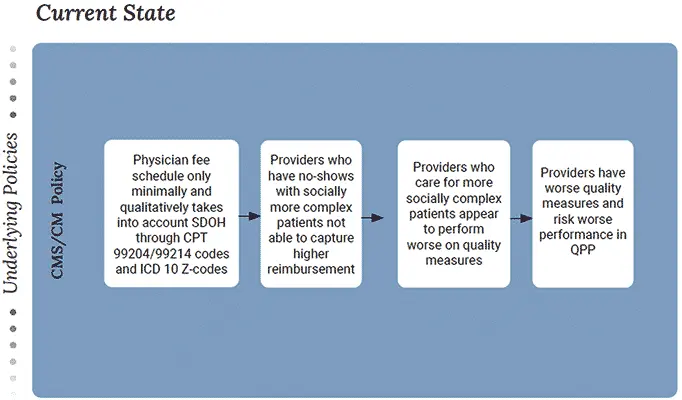
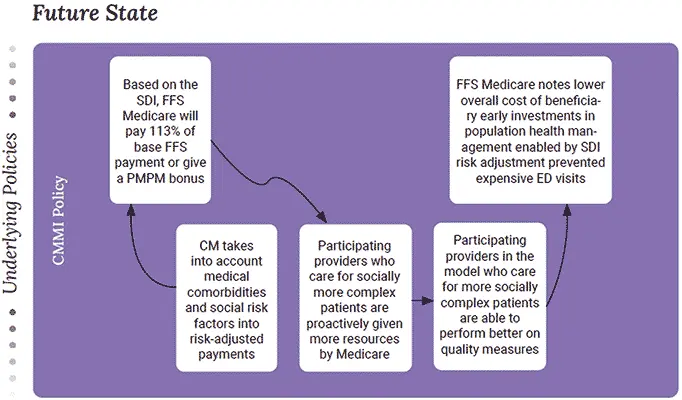
Source: Phillips, Ostrovsky, Bazemore – Workshop on Social Risk Payment Adjustment



